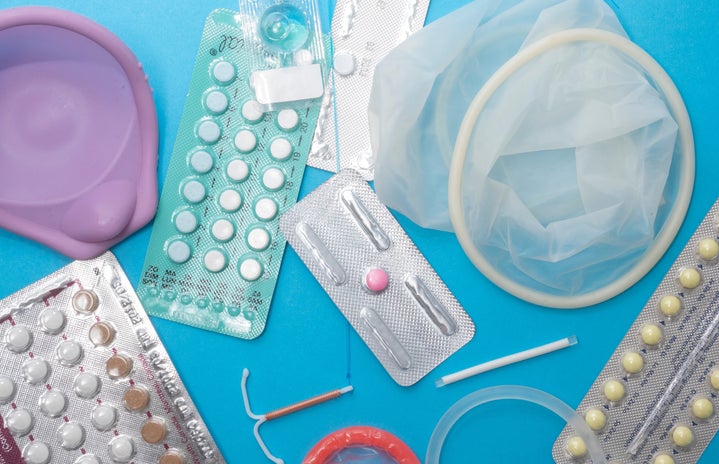
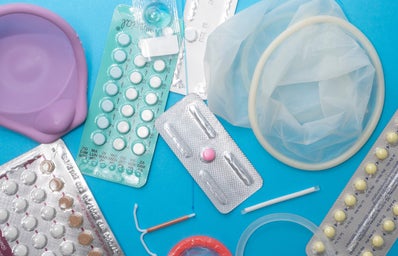
Doug Ford’s recent cuts to OHIP+ offerings, that includes contraceptive coverage, has caused birth control to be a major topic of discussion. Being a sexually active woman myself, I have gone through the process of finding a method of birth control that works for me. Despite being enrolled in a science program here at Western, I still found myself lost when reading some of the literature given to me by my family doctor about my options. It is so important for women, especially young women, to take control of their sexual health. However, we aren’t always given the resources to do so.
Below I have listed some birth control options and how they work.
Oral Contraceptives
Oral contraceptives are by far the most popular form of birth control. Despite their prevalence, they are not as simple as they appear. There are three different types of oral contraceptives: combined hormone pill, progesterone only, and the extended use pill. The difference between these oral contraceptives is their hormonal composition and how they manage your cycle.

Combined Hormone Pill & Progesterone Pill
The combined pill is a mixture of hormones progesterone and estrogen whereas the progesterone pills only contain progesterone. Progesterone hormone is the main active ingredient in this form of birth control. It works by preventing ovulation. Ovulation is when an egg is released from your ovary into the fallopian tube where it can be fertilized by sperm. If you don’t release an egg, you cannot get pregnant. Progesterone also decreases the likelihood that sperm will be able to reach the region of fertilization (fallopian tube) by making the mucus in your vaginal canal harmful to them.
Extended Use Composition
Extended use composition is also known as ‘seasonale birth control’. This method of oral contraceptives works the same way as the combined and progesterone pill, the only difference is the pattern in which you take them. Instead of having a period every month, the hormone pills extend for three months and there is one set of sugar pills at the end of the third month. You may be thinking “Oh my god that would be great to only get my period every 3 months, I need to give that a try!”. Before you head to your family physician and ask for this method of birth control there are a few things to consider. First, it is very healthy for your uterus to have a period every month as part of your cycle. The reason for this is missing periods consistently for a long period of time can increase your risk of endometrial cancer because you aren’t shedding your uterine lining. Women who are prescribed this form of birth control are typically experiencing challenges regulating their period or are having extremely irregular periods.
Things to consider. . .
-
The birth control pills only work if you are dedicated to their use. This means taking them consistently and at the same time. Don’t panic if you miss one, you simply take it when you remember to take it. If you miss a dose, it is suggested that you don’t have sex for at least 24 hours.
-
There are issues associated with inconsistent use of the pill which means it is crucial to have a consistent schedule.
-
If you take your pill at irregular times regularly you may experience:
-
Abnormal bleeding
-
Nausea
-
Breast tenderness
-
Pregnancy risk is 3x higher
-
Excessive hair growth on the face, chest and back
-
-
-
If you aren’t feeling well while taking your newly prescribed birth control, it is possible the formulation doesn’t work for you and you can request to try a different one.
-
Approximately 9% of women taking the pill will become pregnant
-
For the pill to effectively prevent ovulation and provide ample protection against pregnancy you must take the pill for three months. During these first three months condoms are necessary to prevent pregnancy.
-
To decrease your chances of pregnancy even further, it is suggested that condoms are used with birth control pills.
-
You cannot smoke cigarettes while using birth control because of an increased risk of stroke.
-
Birth control can be used to help acne through hormone regulation. There are specific brands for helping with acne.
-
In some women the pill can cause weight gain but there is no conclusive evidence about this.
-
It is rare, but some women develop strong mood swings and depression.
Intrauterine Devices (IUD)
There are two main kinds of IUD’s: copper and hormonal. The IUD is a copper wire that is inserted into your uterus through your vagina at your family doctor’s office or a gynaecologists office. IUDs have the highest effectiveness rating of 99%.
Copper IUD
The copper IUD works through acting as a local spermicide in the uterus. This means that it destroys the sperm before it can reach the fallopian tube where it can fertilize an egg. If sperm reaches the fallopian tube, the copper IUD has a backup way to prevent pregnancy. It is shaped like a T and this shape allows it to rub against the lining of the uterus which prevents the buildup of the uterine lining and makes your uterus an unwelcoming home for a fertilized egg.
Copper IUDs typically increase the amount that you bleed every month and can cause worse cramps. These side effects are most significant in the first 3-6 months after implantation and may improve over time. Other side effects include spotting between periods, irregular periods, longer or heavier periods, and more or worse cramping during periods. The only real benefit of copper IUDs over hormonal IUDs is that you do not have any of the risks associated with all forms of hormonal birth control.

Hormonal IUDs work in two ways. The first being that through releasing hormones in the uterus, it thickens the mucus at the cervix. The thicker the cervical mucus the more difficult it is for sperm to travel through and fertilize an egg. The hormones released from the IUD itself work similarly to the oral birth control and work to stop ovulation so there is no egg released that can be fertilized. One major benefit of the hormonal IUD is that the hormones are released within your uterus and they do not have to be processed by your liver. This is extremely beneficial if you are someone who has to take lots of other medications that can be taxing on your liver.
Hormonal IUDs can have some side effects, most being very mild. Most women describe that after 6 months they have much lighter periods, while some women report their periods stopping completely. Missing your period when having an IUD is healthy because the device regulates your uterine lining as if you are shedding it every month as a period. Hormonal IUDs can be used to help with symptoms of endometriosis and polycystic ovary syndrome (PCOS). Within the first 3-6 months of having the IUD implanted it is normal to experience some cramping, light spotting, and irregular periods.

Things to consider. . .
-
With an IUD you don’t have to remember to take a pill and you are always protected against pregnancy
-
IUDs can be used for an extended period of time but can be removed at any point
-
Hormonal IUDs are good for 3-5 years
-
Copper IUDs are good for 7-12 years
-
-
There is risk associated with it like taking any other medication.
-
If you use a menstrual cup during your period, most IUDs are not compatible with the use of a menstrual cup.
-
IUDs can be very expensive without coverage with a one time fee around 415 CAD.
-
No risk of stroke due to smoking cigarettes while using an IUD.
NuvaRing
NuvaRing is a relatively new form of birth control. NuvaRing is a silicon ring that you insert into your vagina so that it sits at your cervix. It contains a mixture of progesterone and estrogen similar to the combination birth control pill. That means it works by preventing ovulation.
NuvaRing is used in a cycle. After insertion, it can be left in your vagina for up to 3 weeks. At the third week mark you are to remove it so that you can have a period. When your period is finished you have to insert a new NuvaRing. With proper use and insertion, NuvaRing can be 98% effective in preventing pregnancy.
Side effects to consider before using NuvaRing is that some women experience irritation of the vagina and cervix where NuvaRing sits. Other side effects are headaches, nausea, mood swings, painful menstrual periods and less sexual desire.

Things to consider…
-
You cannot smoke cigarettes while using NuvaRing.
-
You have to purchase a new NuvaRing every month and they are about 30 CAD.
-
Typically not covered by health benefits.
-
You need to stick to a very strict schedule, meaning NuvaRing should be removed and inserted at the same time each month in order to have maximal effect.
-
When life gets busy this could be challenging and you may leave yourself vulnerable.
-
-
Navigating penetrative sex with a NuvaRing is considered a non event.
-
If you have placed the NuvaRing where it is supposed to be (at your cervix) you should not feel it and neither should your partner.
-
If it is in the correct location it will stay in place during intercourse.
-
Contraceptive Patches
The only contraceptive patch that is currently available in Canada is called Evra. Evra is a sticky patch worn on the skin. The patch contains two hormones: synthetic versions of estrogen and progesterone to prevent ovulation. It also makes cervical mucus thicker which impedes sperm’s swimming. The patch is worn for 3 weeks every month, however, every 7 days you must replace the patch. It is recommended that you never are without a patch for longer than 7 days and that the patch is removed on the same day every month. The side effects of this form of birth control are very similar to the other hormonal birth controls already mentioned.

-
You cannot smoke cigarettes while using a contraceptive patch.
-
Each patch is approximately 12 CAD, so every month it costs 36 CAD.
Spermicides

Spermicides are exactly what they sound like. They are chemicals put in your vagina before sex that kill and harm sperm so they are unable to fertilize an egg. It does this in two ways, the first being it blocks your cervix and the second being it impedes sperm’s ability to swim. Spermicides can be used on their own, however it is recommended that they are used with other birth control methods like the male or female condom. When used individually, spermicides are only 72% effective when it comes to preventing pregnancy. Spermicides contain certain chemicals that may irritate the vagina.
A note on emergency contraceptives:
Plan B, nicknamed the ‘morning-after pill’, can be used after you engage in unprotected sex. Ideally the pill is taken within 3 days of unprotected sex, as for every day that follows the effectiveness of the pill decreases. However, Plan B can be effective up to 5 days after sex. Do not take more than one dose of the morning after pill.
After taking the pill, you may experience some light cramping and very light spotting. Your first period after taking the morning after pill will be different than what you normally experience and that is normal. If you throw up 2 hours or less after taking the pill it will not work and is recommended you take another dose. Lastly, Plan B is very expensive in Canada. Each pill is 35-40 CAD per pill so it is not a method that should be relied upon often.
All of the above forms of birth control protect against pregnancy and not STIs. The best way to prevent the transmission of STI’s is to use a male condom or female condom when engaging in penetrative sex. If engaging in oral sex the male condom is also effective for men and for females a dental dam can be used.

DepoProvera
DepoProvera is a form of birth control shot administered every three months. It contains a synthetic hormone that resembles progesterone and protects against pregnancy. It has a 88-94% effectiveness. DepoProvera is not the number one choice recommended by doctors due to a multitude of side effects. The most concerning of these side effects being potential bone thinning that puts women at greater risk for developing osteoporosis in the future. Osteoporosis is a bone disease where there is major reduction in bone density that increases the risk of fractures. The risk of osteoporosis is even greater if DepoProvera is used until menopause. Other serious side effects include severe depression, migraines with aura, very heavy bleeding for extended amounts of time, and yellowing of the skin or eyes. I’ve simply included this method to be thorough and I strongly advise you not to choose this method.
Resources for funding birth control
As I mentioned before, Doug Ford cutting OHIP+ offerings has removed funding for birth control and other prescription drugs if you have any other form of health insurance. However, as Western students, we are lucky because if you opt into the student health plan 80% of charges associated with prescription drugs are covered. You can search your prescription drug here to make sure it is covered here.
Here is a list of the above methods and their coverage status under the UWO Student Health Plan:
Oral contraceptives—Yes, you can search your specific drug at the link above.
Hormonal IUD Kyleena—Covered
Hormonal IUD Jaydess—Covered
Hormonal IUD Mirena—Covered
Copper IUD Liberte/ParaGard—Not covered
DepoProvera—Covered
NuvaRing—Covered
Evra Patch—Covered
Spermicides—Not covered
This information is accurate as of January 6th, 2021. If the drug you require is not covered you can download a ‘Drug Exception Form’ and make a case for coverage.
If you have opted out of the student health plan for any reason, you still have options. In London, there are birth control clinics that offer reduced costs for all birth control services that are under the regulation by the Middlesex-London Health Unit. This is a link to their services that includes a list of reduced prices. If you are not located in London, birth control clinics are located in most major cities in Canada.You can locate them by searching birth control clinics online followed by your nearest city’s name. If one of these birth control clinics is not available to you explore your options with OHIP+ if you have no other health coverage.
The best advice I can give when trying to find the birth control that works for you is do your own research, establish what you’re comfortable with and don’t be afraid to ask your doctor questions. That is what they are there for!
Related Articles
Want more HCW? Check us out on social media!
Facebook, Twitter, Instagram, Pinterest
Subscribe to our newsletter!