As we exit 2020 with Covid-19 still running rampant in the United States, many of us have gotten used to a “new normal”. Case numbers continue to rise and with socially distant classes, new business hours, and enforced building capacities, we cannot help but to reevaluate seemingly simple parts of our day to day lives. Healthcare workers have constantly had to face the brunt of these changes. Overcrowded hospitals, long hours, dwindling beds, and waning single use supplies turned long-term protection measures are just a few of the things frontline workers have experienced during the pandemic. I recently got the chance to conduct a short interview with one of my friends who is a nurse. I wanted to ask her questions and give her an opportunity to give us personal insight into her job, but more importantly aspects of that job that have changed since the first few months of 2020. Here is what she had to say…
Emily: “So what has been the scariest part of being in healthcare during a pandemic?”
Raven: “I would honestly have to say that the scariest part of it is the fear of the unknown. Any patient we come in contact with could be positive. We have to trust that our patients are disclosing their symptoms [past and current] properly and trust that they are disclosing any positive test results. It also isn’t just the fear of yourself being exposed, it’s the invisible transmission to your family and coworkers too.”
Emily: “Can you run me through a timeline of your shift in the hospital or working with Covid-19 patients?”
Raven: “So I work in the OB/GYN unit of the hospital. We don’t always have Covid-19 patients, but we have had to work with them”. (She then disclosed that if hospitals were short or overcrowded personnel would be transferred around floors for their shift. Coincidentally, this had just happened to her and she worked a shift on the floor with Covid-19 patients.) “Each patient has a cart outside of their room with our PPE on it and in every room we have to set up where they have their own vital sign machine, computer for meds, and any other equipment we might need. We are allowed to take care of four Covid patients at a time. When I first arrive, I get reports and then check all orders. Then, I will call into each room checking to see if the patients need anything and ensuring they are comfortable. After that, I gather all supplies before gowning up. After gowning up I make my first rounds to do my full assessments, discussing care plans, and any teaching. [All of the patient’s] rooms are usually side by side, so we have to use the same PPE because of the shortage. We have to do our rounds every four hours in order to further limit personal and secondhand exposure and we try to ensure all check ins are done for the same amount of time [each time]. We are also given hospital scrubs to change into for the duration of our shift and we are told to separate ourselves from the other nurses that are on the same shift, so we do not contaminate them. Also, we are not allowed to assist in anything outside of that unit; anything that involves going into a non-Covid room is off limits.”
Emily: “The dressing process alone seems like a lot, especially when we think about the shortage of proper supplies for people on the frontline. Can you tell me more about what that process looks like? Can you attest to the ‘wearing multiple masks at a time’ thing?”
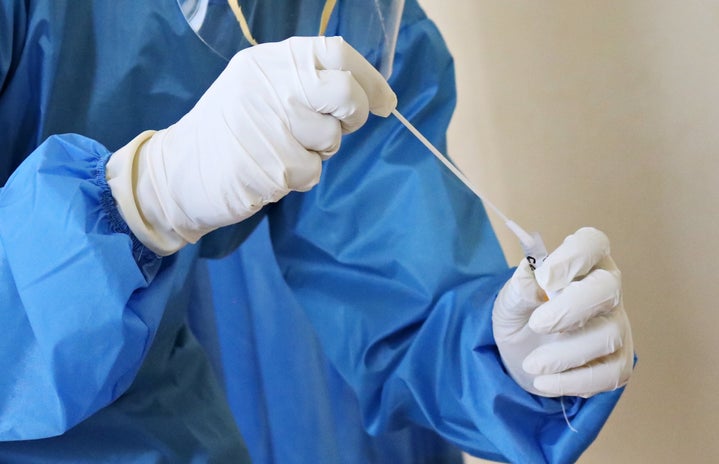
R: (She laughs about the masks) Yeah, we have definitely had to layer masks on multiple occasions. Not as much anymore thankfully! As for the dressing process: after washing up and sanitizing, the first thing we get to do is put on our gowns, they are full length hospital scrubs over our regular scrubs. Our masks are next, they are N95s and we always pay careful attention to this. We have to have a proper seal and ensure that we cannot smell anything. Next, we get goggles and a face shield. Finally, we put on our gloves and we are ready!”
Emily: “How about undressing?”
(We laugh at the absurdity of this question)
R: We are given one mask per shift, so once we leave the room, we have to take it off and place it in a paper bag. We remove the face shields next and wipe down the inside and outside for our later usage. We store them in a bag also, then we finally wash our hands. Everything has to be very precise and we have to limit pretty much any contact with anything on ourselves or anything that others could even come in contact with. It is all a very careful process.
Emily: “What is the energy like in your hospital?”
R: Stressed. The floor [OB/GYN] that I am usually on has to be extra careful because of the newborns and mothers. We have to be a lot more careful about exposure from everyone basically. The mothers are there recovering too, and it is just as important for them. Also, there’s the fact that a lot more nurses are getting sick, so we are usually working short staffed.”
Emily: “Have your habits changed any? Inside and outside of the hospital?”
R: “Honestly, not a lot has changed in the hospital [with cleaning]. We have to wear masks for 12+ hours no matter what!” She then talks about how they are a regular part of everyone’s unform, including patients, regardless of where that person is working or what their title is in the hospital. “We already wiped down workstations and equipment before, during, and after shifts. As for outside of the hospital, my habits have definitely changed! It is things that many of us are doing, but I do feel like I pay special attention to it now. Or maybe it is just more prevalent to me because of work. Masks everywhere and hand sanitizer is used everywhere after everything. I also carry wipes for things like gas pumps, grocery carts, things like that before I touch them.”
Emily: “The shortage of protection and equipment has always been heavy on my mind. You guys are directly exposed and getting hit hardest. Has any of this changed your view of the medical field? Is it good or bad?”
R: “Well…it is a little bit of both. My respect for everyone in healthcare has gone up. I feel like we risk a lot just by showing up for work. And its not just our personal health, but the health and safety of our friends, family, and coworkers. I chose this field because it is my passion and I want to help others; I think it might just be the price we pay? The pandemic is something no one could have predicted but we are trying to do our best with what little we have been given and what little we know.
Emily: “How are healthcare workers being received by others? I feel like the image has been twisted since mask mandates and all?”
R: I have personally received both praise and disgust. I work nights [7pm-7am] so sometimes I will run errands before work, like getting food or a coffee first and I’m obviously in uniform, mask included. There have been numerous occasions where I get praise or a “thank you” but then there are occasions where people get nasty. They try to say things about how I should not be out spreading the disease to others, even when I’m in a mask or before my shift entirely. Its bizarre. The worst part is that these kinds of comments come from people who are out and about but NOT wearing a mask! It is just crazy to me.
Emily: “Okay, so to wrap up I have one more question. What is one thing you would wish others would do or something you wish others understood after working through a pandemic?”
R: “I think I would just ask others to take proper precautions and always be honest with others…including their healthcare providers! Taking precautions is just about being kind and spreading something positive during a pandemic. Also, honesty helps us, and it helps patients. We can treat you appropriately and get you what you need and when you need it, but that honesty goes beyond just keeping frontline workers safe. It is people’s family and friends also that count on that honesty and security.